In my previous blog, I discussed how LTACHs have been slow to improve care coordination and reduce readmissions. I said that only aggressive action towards in-house care coordination could ensure the long-term survival of your business while significantly improving outcomes for your patients.
But what, really, is care coordination? And how do you achieve it?
The term is used frequently, but very few can offer a clear definition, or describe discrete steps to accomplish it. Without a clear understanding of the term, it runs the risk of becoming just another meaningless buzzword.
The official definition of care coordination is the deliberate organization of patient care activities between two or more participants (including the patient) involved in a patient’s care to facilitate the appropriate delivery of health care services. Organizing care involves the marshalling of personnel and other resources needed to carry out all required patient care activities and is often managed by the exchange of information among participants responsible for different aspects of care.
Translation: coordinated care is really just a fancy term for improved communication.
The key to coordinated care is improved communication across the care continuum. When caregivers at different points of care have access to detailed, complete documentation, they are able to make more effective clinical decisions. On the other end of the spectrum, this detailed documentation then has positive impacts on reimbursement processes, reducing AR days and increasing overall revenue.
The business team – coders and billers – must be able to provide feedback if documentation is missing or incomplete. When they are dealing with a stack of paper forms with multiple serious errors – or, worse, a stack of paper forms with only one serious error – they then must trace down the clinician to have them correct the error(s). This may involve a series of emails, scans, faxes, or phone calls, each of which take significant amounts of time. And then the claim gets denied by Medicare. Lather, rinse, repeat.
This feedback loop shrinks dramatically when coders, billers, and practitioners all fully understand guidelines, processes, and procedures.
Except that there are mountains of procedures, not to mention the many thousands practitioners don’t have the time or the bandwidth to follow them.
Unsurprisingly, the secret to coordinated care is integrated health technologies that facilitate and improve communication between teams.
I know. Shocker. But bear with me.
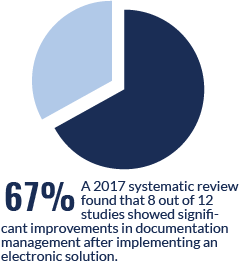
Source: 2016 CAQH INDEX: A Report of Healthcare Industry Adoption of Electronic Business Transactions and Cost Savings.
Let’s use LTACH pre-admission screening as an example. At Cantata Health, spent over five years developing a pre-admission screening portal in partnership with our clients, ensuring that the technology was tailor-made to the needs of LTACH pre-admission procedures.
But you don’t have to use Cantata Health products to achieve coordinated care (don’t get me wrong, we would certainly like it if you did). But there are some features you should look for when evaluating an electronic health solution that will actually facilitate coordinated care.
Coordinated Care Solutions Should Be Web Based
Web based electronic health solutions allow practitioners to conduct screenings and complete documentation in real time. Returning to the pre-screening portal example, our web based screening documentation can be ready for financial review in three easy steps on a tablet or laptop as your liaisons go about their tasks. This allows them to focus on the relevant conversations, data, and metrics that they need to complete their documentation.
While the increased mobility is a huge benefit, web based solutions are becoming increasingly more common with the steady migration to cloud-based technologies. And as demand for healthcare continues to increase, this transition will only accelerate in the coming years.
Coordinated Care Solutions Should Be Integrated
I know I said “integrated” before, but I really mean it. There’s no reason to fill out the same information multiple times on electronic forms. That’s why our pre-admission portal integrates seamlessly with our EHR and RCM software. Any demographic information entered during the pre-admission process is automatically compiled and uploaded into your EHR and RCM tools, not only ensuring that any and all forms are completed correctly, but also eliminating redundancies in a practitioner’s routine.
Integration also prevents mistakes or inaccuracies across forms that may impede payment processes or, worse, compromise patient care. Which brings me to my next point.
Coordinated Care Solutions Should Be Real Time
If a pre-admission liaison completes a the pre-admission process, the resulting forms should be available to the coding and billing team for immediate review. This way they can identify and flag inconsistencies and then… wait for it… communicate them back to the liaison so that they can address these concerns, often prior to leaving the acute care facility. Closing this feedback loop rapidly accelerates the admission process, getting patients to the care they need faster.
Coordinated Care Solutions Should Be Data Centric
Not only should coders and billers be able to access pre-admission forms in real time, they should also have detailed analytical history about the referring physician, clinical indicators, and number of referrals. That’s why our product includes an analytics dashboard, allowing a broader view to improve high-level business decisions that in turn improve the overall function of your organization.
These types of data based decisions are extremely important now, but will become even more essential as the healthcare industry transitions to payment for care quality and overall cost effectiveness.
